Staphylococcal Infections
Staphylococcal (stah-fih-lo-KAH-kul) infections are infections caused by Staphylococcus aureus (stah-fih-lo-KAH-kus ARE-ree-us) and related species of bacteria.
KEYWORDS
for searching the Internet and other reference sources
Antibiotic resistance
Cellulitis
Food poisoning
Impetigo
Methicillin-resistant staphylococcus aureus (MRSA)
Scalded skin syndrome
Staphylococcus aureus
Toxic shock syndrome
Vancomycin Intermediate staphylococcus aureus (VISA)
What Are Staphylococcal Infections?
They cannot be seen with the naked eye, but bacteria cover the skin's surface. Staphylococcus aureus bacteria, also called staph bacteria, often live on people's skin, particularly around openings such as the nose, mouth, genitals * , and rectum * and sometimes inside the nose and mouth, without causing disease. But when a person's skin is broken or cut, the bacteria can enter the wound and cause an infection. Staph infections range from minor skin infections to joint, bone, or lung infections to widespread or systemic infections. Some strains * of staph produce a toxin (or poison) that causes illness.
Newborns, elderly people, and people with immune systems weakened by diseases such as cancer and AIDS * are at greater risk of serious staph infections. Some serious infections can be acquired in a hospital when a patient is being treated for another condition.
How Common Are They?
Some species of staph bacteria are present on people's skin all the time. The more dangerous Staphylococcus aureus may come and go regularly from people's noses and skin. Skin infections caused by staph, such as boils, are quite common. Many staph infections are minor and do not require treatment; serious staph infections are less common.
* genitals (JEH-nih-tuls) are the external sexual organs.
* rectum is the final portion of the large intestine, connecting the colon to the anus.
* strains are various subtypes of organisms, such as viruses or bacteria.
* AIDS, or acquired immunodeficiency (ih-myoo-no-dih-FIH-shen-see) syndrome, is an infection that severely weakens the immune system; It is caused by the human immunodeficiency virus (HIV).
Are They Contagious?
Sometimes staph infections of the skin are contagious. If a person touches another person who has a staph infection of the skin and then touches his or her own mouth or nose or an area of broken skin, the staph infection can spread. A person also can spread the bacteria from one part of the body to another through touch. Staph can be transmitted via contaminated surfaces and food and through the air as well.
What Are Some Types of Staph Infections?
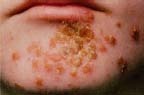
Impetigo (im-pih-TEE-go) is a skin infection that usually occurs around the nose and mouth. In impetigo, fluid-filled blisters develop and often burst and form yellowish crusts. Impetigo is a contagious infection that can spread if a person scratches the blisters and then scratches or touches another area of the body.
Carbuncles (KAR-bung-kulz) and furuncles (FYOOR-ung-kulz), also known as boils, are staph infections that produce a red, swollen bump filled with pus * in the skin surrounding a hair follicle * . With boils pus forms in a single hair follicle, whereas carbuncles form from grouped furuncles and have several small chambers, like a series of connected boils.
Cellulitis (sel-yoo-LYE-tis) is an infection of the deeper layers of the skin and the connective tissues below the skin's surface. People with cellulitis usually have an area of red, swollen, tender, warm skin. They also may have fever, swollen lymph nodes * , and a general feeling of illness. Cellulitis is most common on the face and lower legs.
Scalded skin syndrome (also known as Ritter disease) is a staph infection that typically occurs in infants and children less than 5 years old and causes large portions of skin to be shed from the body. In this condition the staph bacteria produce a toxin that damages skin. Fluid collects beneath the skin and loosens it so that large portions slip off when rubbed. When the skin slips off, it leaves raw areas that eventually crust over. When the area under the skin is exposed, the child is at risk of excessive fluid loss and additional bacterial infections. Other symptoms include fever and skin redness and tenderness. Babies with this condition may become extremely ill.
Toxic shock syndrome (TSS) is a severe infection that, like scalded skin syndrome, is caused by a toxin produced by staph bacteria. It was first recognized in the late 1970s and early 1980s, mostly among women who were using certain types of very absorbent tampons, but it can occur in people of both sexes and in both children and adults. Because this type of absorbent tampon is no longer available, TSS now usually develops after surgery or in wounds that, in most cases, do not look infected but contain the toxin-producing staph. Skin abscesses * or other staphylococcal infections also may lead to TSS. Symptoms of TSS include sudden fever, low blood pressure, very red rash, vomiting, diarrhea (dye-uh-REE-uh), and muscle pain.
Staph bacteria can produce other types of toxins that cause food poisoning if a person eats contaminated food (usually meats, poultry, eggs, and dairy products) that has not been heated or refrigerated at the proper temperature. Symptoms include belly pain, nausea (NAW-zee-uh), and vomiting. If the food poisoning is severe, a person may experience headaches, muscle aches, and blood pressure changes.
The Evolution of
Antibiotic-Resistant
Staph
Antibiotics are used widely to treat infections such as those caused by staph. Over time, staph bacteria may become stronger so that the antibiotics may not be as effective against the germ, which is known as antibiotic resistance. When Alexander Fleming discovered penicillin in 1928, staph bacteria were highly sensitive to it. Now, few staph bacteria are killed by penicillin. These bacteria often are resistant to many antibiotics. The more important strains of antibiotic-resistant staph are known as methicillin-resistant staphylococcus aureus (MRSA). MRSA is resistant to commonplace antibiotics, but it is still susceptible to the last-resort, more powerful medications. A more serious strain of staph infection, vancomycin intermediate staphylococcus aureus (VISA), can resist vancomycin, one of the most powerful (and last-resort) antibiotics available. Although all strains of the bacteria found so far have been treatable with some type of antibiotic, VISA potentially could defy all medication currently available to treat such infections. MRSA and VISA infections usually develop only in a hospital or health care facility, where prolonged treatment of patients with several antibiotics is common.
* pus is a thick, creamy fluid, usually yellow or greenish in color, that forms at the site of an infection. Pus contains infection-fighting white cells and other substances.
* hair follicle (FAH-lih-kul) is the skin structure from which hair develops and grows.
Some staph infections affect internal organs. Staph is a common cause of the bone infection osteomyelitis (ah-stee-o-my-uh-LYE-tis). Staph infections also may cause pneumonia (nu-MO-nyah), an inflammation of the lungs; blood infection (sepsis); and, more rarely, meningitis (mehnin-JY-tis), an inflammation of the membranes that surround the brain and the spinal cord (the meninges, meh-NIN-jeez). The bacteria may spread from an infection elsewhere in the body, or they can come from a medical device, such as a catheter * , that has been colonized * by staph bacteria. Staphylococcus aureus also may infect the heart valves, where it causes inflammation and gives rise to a condition called endocarditis (endo-kar-DYE-tis).
How Is a Staph Infection Diagnosed?
A doctor may diagnose and treat a staph infection based on its appearance, but a definite diagnosis is made by identifying the organism under a microscope or by culture * . Samples are taken from the site of the infection, which may be the skin, the blood, or an abscess. Staph food poisoning generally is diagnosed based on symptoms, dietary history, and sometimes illness in other people who have eaten the same food or eaten at the same place.
What Is the Treatment for Staph Infections?
Minor skin infections caused by staph bacteria often can be treated with an over-the-counter antibiotic ointment, or they can heal on their own. If a person has an abscess that stems from a staph infection, surgery to drain the pus may be necessary in addition to antibiotics, to allow the infection to heal.
More serious staph infections, such as endocarditis, osteomyelitis, TSS, and scalded skin syndrome, usually require hospitalization and supportive care, such as antibiotics, intravenous fluids to prevent dehydration, and other medications. Endocarditis caused by staph may require surgery in which the infected, damaged heart valve is removed and an artificial valve is inserted.
Because antibiotics are used widely to treat both minor and serious infections caused by staph and other bacteria, some strains of bacteria have become resistant to common antibiotics. New medications and forms of treatment will be important in the future, and scientists are working to develop a Staphylococcus aureus vaccine that might help people with weakened immune systems resist staph infection.
How Long Does Infection Last?
Minor skin infections caused by staph bacteria usually clear up within a week, whereas more serious widespread illnesses may take several weeks to more than a month to get better.
* lymph (LIMF) nodes are small, bean-shaped masses of tissue that contain immune system cells that fight harmful microorganisms. Lymph nodes may swell during infections.
* abscesses (AB-seh-sez) are localized or walled off accumulations of pus caused by infection that can occur anywhere within the body.
* catheter (KAH-thuh-ter) is a small plastic tube placed through a body opening into an organ (such as the bladder) or through the skin directly into a blood vessel. It is used to give fluids to or drain fluids from a person.
* colonized means that a group of organisms, particularly bacteria, are living on or inside the body without causing symptoms of infection.
* culture (KUL-chur) is a test in which a sample of fluid or tissue from the body is placed in a dish containing material that supports the growth of certain organisms. Typically, within days the organisms will grow and can be identified.
What Are the Complications of Staph Infection?
Minor staph skin infections rarely result in complications, but some can produce more widespread infection, such as sepsis, a serious systemic infection caused by bacteria invading the bloodstream. TSS can lead to shock * , organ failure, and death. Scalded skin syndrome can give rise to other infections, dehydration, and sepsis. Osteomyelitis can cause permanent bone damage and may require surgical treatment.
Can Staph Infections Be Prevented?
There are several ways to help prevent the spread of staph infections:
- washing hands before eating and after using the toilet, or touching the nose
- washing any cuts, scrapes, or open sores
- keeping wounds covered with a clean bandage
Food poisoning can be prevented by washing hands before food preparation, storing food properly before cooking, cooking food to the appropriate temperatures, using clean utensils and dishes, and refrigerating or freezing food as soon as possible after cooking. To lessen the risk of TSS, women are advised to use less-absorbent tampons, to change them frequently, and not to use only tampons during a menstrual period, or to avoid tampons altogether.
* shock is a serious condition in which blood pressure is very low and not enough blood flows to the body's organs and tissues. Untreated, shock may result in death.
Resource
Organization
U.S. Centers for Disease Control and Prevention (CDC), 1600 Clifton
Road, Atlanta, GA 30333. The CDC provides information about infections
such as staph, how often they occur, and how to prevent them.
Telephone 800-311-3435
http://www.cdc.gov
taking the 1st 2 antibiotics. I ended up in tbe ER after 8 weeks of pain, swelling, redness, stiffness, and suffering! I then was prescribed Keflex in the ER for 10 days, 3x a day. Im finished my meds, and its NOT gone away yet! I still have it on my shin to my foot, glassy, yellowish, tight stretched feeling, and red dots scattered around, still reddish slightly around the whole lower leg also, still pain in my foot, toes, ankle and calf when i walk too. Dr did not give me anymore meds at my follow up, HELP! Do i need more meds to get rid of this thing completely?? Or will it go away on its own now after taking the round of antibiotics? Its awful and i really want it gone!! Going back to another primary for 2nd opinion in a few days. I need answers! This is so frustrating!