Skin and Soft Tissue Infections
Skin and soft tissue infections are infections involving the layers of the skin and the soft tissues beneath it.
What Causes Skin and Soft Tissue Infections?
Viruses, bacteria, and fungi generally cause skin and soft tissue infections by entering the body at a spot where a cut, scrape, bite, or other wound has broken the skin; some infections are even the result of bacteria that normally live on the body. These infections can affect the layers of the skin or deeper tissues, such as muscle and connective tissue (the interlacing framework of tissue that forms ligaments, tendons, and other supporting structures of the body), and they may bring about symptoms in other parts of the body.
KEYWORDS
for searching the Internet and other reference sources
Abscesses
Boils
Carbuncles
Cellulitis
Dermatology
Dermatophytes
Furuncles
Impetigo
Molluscum contaglosum
Necrotizing fascitis
Ringworm
Tinea
Warts
Many infections like varicella (chicken pox) and measles (rubeola) affect the skin, but these infections involve the whole body and do not primarily arise within the skin or soft tissues.
What Are Some Types of Skin and
Soft Tissue Infections?
Dermatophyte infections
Dermatophytes (dur-MAH-toh-fites) are fungi that live on the dead outer layer of skin. Sometimes they can produce symptoms of infection. Tinea (TIH-nee-uh) infections, commonly called ringworm (although they have nothing to do with worms), usually are caused by the Trichophyton group of these organisms. They include tinea pedis (PEE-dis), or athlete's foot; tinea cruris (KRU-ris), or jock itch; tinea capitis (KAH-pih-tis), or ringworm of the scalp; tinea unguium (UN-gwee-um), or ringworm of the nails; and tinea corporis (KOR-poorus), or ringworm of the body. Damaged skin is more vulnerable to infection, as is skin in warm, moist areas of the body. When the fungus takes hold, it typically causes a ring-like rash of red, flaking skin. The border of the rash may be raised, as if a worm were under the skin. The rash's shape and this raised edge led people to call the infection ringworm. When the nails are infected, they usually become yellow, thickened, and brittle.
Tinea versicolor, or pityriasis (pih-tih-RYE-uh-sis) versicolor, is caused by the fungus Malassezia furjur. Symptoms include scaly patches of skin, ranging in color from light to dark. The patches occur on the chest, neck, back, underarms, and upper arms. Hot, humid weather encourages the growth of tinea versicolor. These fungal skin infections typically are treated with antifungal creams or ointments. In severe cases or when the infections do not improve with this therapy, several antifungal medications are available that may be given by mouth.
Impetigo
Impetigo (im-pih-TEE-go) refers to a skin infection in which there are red blister-like bumps that contain a yellowish fluid or pus * . After the blisters break open, they crust over. Impetigo is most common on the face, especially around the nose and mouth. Usually, either streptococcus (strep-tuh-KAH-kus) or staphylococcus (stah-fih-lo-KAH-kus) bacteria are the cause of the infection. Impetigo can spread easily, especially among children, who may scratch the lesions and then touch other areas of their skin or another person. People also can contract impetigo from handling clothing or blankets that have been in contact with infected skin.
Doctors prescribe antibiotics to treat impetigo. The infection generally clears up without leaving permanent skin damage.
* pus is a thick, creamy fluid, usually yellow or greenish in color, that forms at the site of an infection. Pus contains infection-fighting white cells and other substances.
Skin abscesses
Skin abscesses (AB-seh-sez) may occur in areas of the skin where the body has been fighting a bacterial infection. To isolate the infection, the body forms a wall of tissue around the collection of pus, and this area is the abscess. Abscesses are usually round, raised, and red, and they may feel warm and tender. A furuncle (FYOOR-ungkul), or boil, is an abscess that forms at the base of a hair follicle * . A carbuncle (KAR-bung-kul) forms when the infection spreads to include several follicles and the surrounding skin and deeper tissues. Like furuncles, carbuncles are red, raised, and sore to the touch.
Most skin abscesses eventually burst to allow the pus to drain out, but treatment with antibiotics may be needed to clear up the infection in some cases. Skin abscesses that do not improve on their own need to be lanced (punctured and drained) by a doctor.
Cellulitis
Cellulitis (sel-yoo-LYE-tis) is an inflammation of the skin and/or the tissues beneath it. The culprits behind the infection are almost always group A streptococcus or Staphylococcus aureus (stah-fihlo-KAH-kus ARE-ree-us) bacteria. Cellulitis may occur in people with diabetes * or those who have immune system problems even if they do not have a skin injury. The infection can occur anywhere on the body, but it is found most frequently on the face and lower legs. It appears as tender, red, swollen areas of skin. The skin in the infected area may feel stretched and warm. A few days after the first symptoms, patients may experience fever, chills, and muscle aches. Red streaks also may appear on the skin, signaling the spread of the infection.
Antibiotics are used to treat cellulitis. Even after the infection is gone, the skin may look different for several weeks. Complications are rare, but they can include sepsis * , gangrene * , and lymphangitis * . Cellulitis may involve infection of deeper tissue called the fascia (FAY-she-uh). Infection in this layer can be very serious or even life threatening and often requires surgery to remove the infected tissue.
Necrotizing fasciitis
Necrotizing fasciitis (NEH-kro-tie-zing fashe-EYE-tis), also called flesh-eating disease, is a rare but potentially fatal disease caused by group A streptococcus bacteria infection. It affects the deeper layers of skin and tissues beneath the skin. Necrotizing fasciitis starts with sudden painful swelling and discoloration (red, purple, or bronze) of the skin. Often, the appearance of the affected skin does not reflect how far the infection has spread into the deeper layers of tissue. The disease can spread rapidly, with the infected area growing larger and darker. The ability to feel in the infected area disappears as the skin tissue dies. As the infection quickly progresses, the patient can become very ill. Early treatment with antibiotics and surgery to remove the damaged tissue is extremely important. Recovery may take several months.
* hair follicle (FAH-lih-kul) is the skin structure from which hair develops and grows.
* diabetes (dye-uh-BEE-teez) is a condition in which the body's pancreas does not produce enough insulin or the body cannot use the insulin it makes effectively, resulting in increased levels of sugar in the blood. This can lead to increased urination, dehydration, weight loss, weakness, and a number of other symptoms and complications related to chemical imbalances within the body.
* sepsis is a potentially serious spreading of infection, usually bacterial, through the bloodstream and body.
* gangrene (GANG-green) is the decay or death of living tissue caused by a lack of oxygen supply to the tissue and/or bacterial infection of the tissue.
* lymphangitis (lim-fan-JIE-tis) is inflammation of the lymphatic system, the system that carries lymph through the body. Lymph is a clear fluid that contains white blood cells.
Molluscum contagiosum
Molluscum contagiosum (moh-LUS-kum kon-tay-jee-O-sum), caused by a virus, produces small, solid, dome-shaped bumps on the surface of the skin. They are flesh-colored and pearly with a dimple in the center. The growths are similar to warts. Viruses cause both conditions—poxvirus in the case of molluscum contagiosum and human papillomavirus in the case of warts. Growths can be single, but they most often appear in groups on the trunk, arms, legs, and genitals * and occasionally on the face.
The disease usually clears up by itself over several months, although new growths may arise on the skin if the virus spreads through contact with infected areas. Doctors may recommend home treatment with over-the-counter medications or removal of the growths by freezing, surgery, laser therapy, or acid treatments.
Herpes Simplex Virus
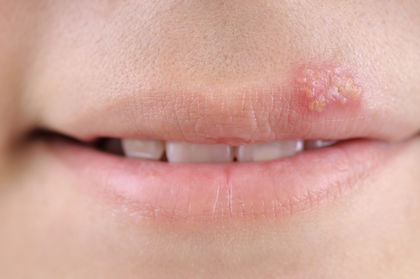
There are two types of the herpes simplex virus (HSV): HSV-1 and HSV-2. Both can show up as skin infections. HSV-1 can cause small, clear blisters (also known as cold sores, fever blisters, or oral herpes) on the face, and HSV-2 can cause blisters in the genital area. These blisters can break, bleed, and crust over, leaving red spots of healing skin.
There is no cure for either HSV-1 or HSV-2. Currently, antiviral medications can help control outbreaks of herpes virus and are used to treat genital herpes or sometimes recurrent cold sores from HSV-1.
Warts
Warts are caused by human papillomavirus (pah-pih-LO-mah-vy-rus), or HPV. They can be skin-colored, pink, tan, or white, and they may appear anywhere on the body. Common warts usually are seen on the hands (especially around the nails), feet, and face, because the virus spreads most easily to those areas. Common warts are rough and raised, but plantar warts, found on the soles of the feet, are flat. Unlike other warts, plantar warts can be painful.
Many warts disappear by themselves after months or even years. Treatments are available for those that do not, including over-the-counter medications or professional treatment by freezing, surgery, laser therapy, or acid treatments.
Are Skin and Soft Tissue Infections Contagious?
Necrotizing fasciitis, cellulitis, and abscesses are not contagious from person to person, but the bacteria that can cause these infections can spread between people. Dermatophytes, warts, and molluscum contagiosum spread fairly easily through skin-to-skin contact.
* genitals (JEH-nih-tuls) are the external sexual organs.
How Are Skin and Soft Tissue Infections
Diagnosed?
A doctor examines the size, shape, and color of the affected area and checks it for tenderness and warmth. The doctor may order blood tests for cellulitis to assess the extent of the infection; tests of skin scrapings for suspected fungal infections or molluscum contagiosum; or tests on a tissue sample for necrotizing fasciitis. Doctors can use a special type of filtered ultraviolet light to check for tinea capitis because the fungi that cause it glow a characteristic color when the light is shined on the infected area.
Can Skin and Soft Tissue Infections
Be Prevented?
The best way to prevent skin and soft tissue infections is to avoid getting cuts, scrapes, bites, or any kind of open wound. Frequent hand washing can curb the spread of bacteria. Doctors also advise keeping any opening in the skin clean and dry. It is wise to consult a doctor if the area around the wound becomes reddened, hot, or painful or if the infected person develops a fever. Dermatophyte infection is best avoided by keeping the skin dry, such as in areas where sweating occurs.
Resources
Organization
American Academy of Dermatology, P.O. Box 4014, Schaumburg, IL 60168.
The American Academy of Dermatology offers fact sheets and general
information about various skin problems on its website. Information for
young people can be found through the Kids' Connection at the
website.
Telephone 847-330-0230
http://www.aad.org
Website
KidsHealth.org
. KidsHealth is a website created by the medical experts of the Nemours
Foundation and is devoted to issues of children's health. It
contains articles on a variety of health topics, including cellulitis,
impetigo, tinea, warts, and other bacterial, fungal, and viral
infections.
http://www.KidsHealth.org